Cardiology 'must be evidence-based' says ACC
The emphasis is on 'wiser healthcare spending'
Ian Mason reports from Chicago

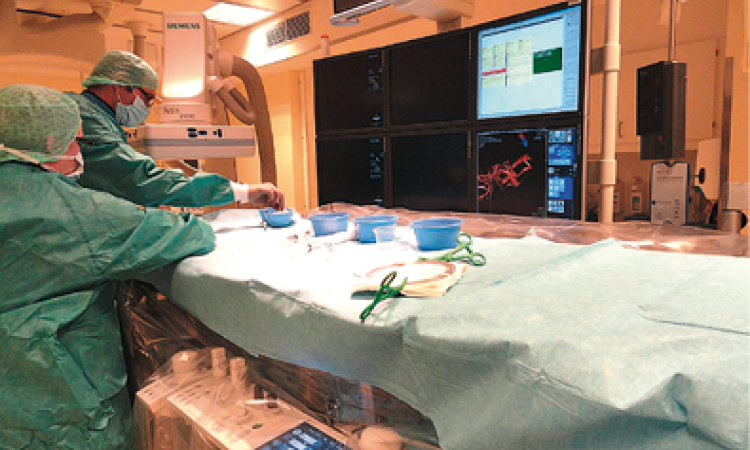
Research by European cardiologists featured in presentations at this year’s American College of Cardiology (ACC) meeting, held in Chicago. Many speakers gave a message equally relevant on both sides of the Atlantic: the need for wiser spending of healthcare budgets.
The ACC keynote opening session set the tone with a snipe at the blockbuster drug Vytorin (ezetimibe/simvastatin). An ACC expert panel recommended that Vytorin should be used only after other cholesterol-lowering drugs have failed. The ACC’s broadside followed disappointing results from the ENHANCE study in which the addition of ezetimibe to simvastatin did not slow progression of atherosclerosis.
The take home message was simple: ‘We need to turn back to statins,’ said Dr Harlan Krumholz, Yale University School of Medicine, who argued that ENHANCE should change clinical practice by encouraging physicians to return to evidence-based medicine – which for him meant more use of statins and less use of ezetimibe.
Elsewhere at the ACC meeting positive evidence was forthcoming; results from the ONTARGET study add the angiotensin II receptor blocker telmisartan (Micardis) to the growing list of cardiovascular drugs with hard clinical end-point data.
Lead investigator Professor Salim Yusuf, McMaster University, Hamilton, Canada, said the results showed telmisartan (80mg/day) to be as effective as the ‘gold standard’ ACE inhibitor ramipril (10mg/day) in reducing the risk of cardiovascular death, myocardial infarction, stroke, and hospitalisation for congestive heart failure in the high risk population studied (over 55 years with coronary heart disease or diabetes).
ONTARGET also examined whether combining telmisartan with ramipril was superior to ramipril alone. Despite the combination lowering blood pressure more than ramipril, there was no additional benefit on the primary end-point, and a higher rate of hypotension-related side effects with the combination.
Treat elderly hypertensives
The Hypertension in the Very Elderly (HYVET) Trial gave a clear answer to the question of whether very elderly people with hypertension can expect the same benefits from blood pressure lowering as younger patients. Treatment with indapamide sustained release (SR) 1.5mg reduced deaths by 21%, fatal strokes by 64% and cardiovascular events by 34%. Lead Investigator Professor Christopher Bulpitt, Imperial College London said the results were good news in light of the growing numbers of people living beyond 80.
‘Elderly individuals with sustained systolic blood pressures of 160 mmHg or more should now be appropriately assessed and treated in accordance with the new findings,’ said Dr Nigel Beckett, the trial coordinator at Imperial College London.
There was further good news for elderly cardiac patients from a study by Dr Nicolas Mansencal and colleagues, Hôpital Universitaire Ambroise Paré, Boulogne, France. Their ten year study of patients aged 80 plus referred to a cath-lab for acute myocardial infarction (MI) showed that although these patients had an early increased risk of mortality, once this acute phase had passed, prognosis at one year was excellent and was comparable with younger patients (Abstract: 1024-78).
Hospital night shift risk to cardiac patients
The hospital night shift may be hazardous for coronary patients, according to a study of 1,650 patients in seven European countries performed by Dr Zbigniew Siudak and colleagues Department of Interventional Cardiology, Krakow, Poland. Their results showed that STelevation myocardial infarction (STEMI) patients treated by primary percutaneous coronary intervention (PPCI) during night hours were less likely to survive compared with identical patients treated during the day shift. Night shift admission was an independent predictor of in-hospital death in multivariate regression analysis model (OR 1.47, 95%CI 1.11-1.94, p=0.007) (Abstract: 1017-54).
Trends in the use of drug eluting stents
The publication of data about risk of late stent thrombosis associated with drug eluting stents (DES) and associated guidance from NICE (National Institute for Health and Clinical Excellence) has led to a significant fall in the use of DES in the UK, according to a study reported by Dr Sunil Nadar and colleagues Gregory Lip City Hospital, Birmingham, UK. However use of DES remains high for complicated lesions such as birfurcation lesions, and chronic total occlusions (Abstract: 1026-143).
30.04.2008