
News • Revealed by AI
Prostate cancer: more than just one disease
Artificial Intelligence has helped scientists reveal a new form of aggressive prostate cancer which could revolutionise how the disease is diagnosed and treated in the future.
Prostate cancer (PCa) is not only one of the most common, but also one of the deadliest types of cancer in men. Diagnostics are correspondingly sophisticated, from imaging via ultrasound or MRI to various biopsy techniques – often even in combination. Keep reading for current developments in early detection, staging, therapy and research.

Artificial Intelligence has helped scientists reveal a new form of aggressive prostate cancer which could revolutionise how the disease is diagnosed and treated in the future.

Targeting a specific protein, Finnish researchers may have found a way to restore drug-resistant neuroendocrine prostate cancer to a state that responds to treatment.
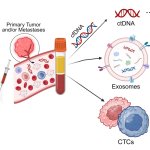
US researchers discuss three blood-based liquid biopsies, namely circulating tumor cells, circulating tumor DNA and tumor-derived exosomes, as they relate to prostate cancer management.
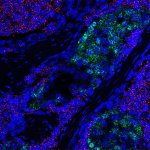
In a new study, UCLA researchers demonstrated how small cell neuroendocrine prostate cancer tumor cells can arise from less aggressive prostate tumors.
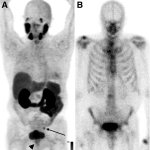
Bone scans have been found to overstage prostate cancer at initial staging compared to prostate specific membrane antigen (PSMA) PET, according to new research.
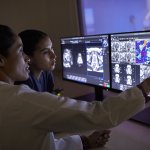
Philips and Quibim have signed a multi-year agreement to work on an integrated solution including an AI-based software to automate real-time prostate gland segmentation in MR images.
Cancer has become strikingly more common in people under 50 in the past three decades, an international research team finds. The reseachers explore what this means for future death tolls.

Combining ultrasound and MRI technology can help detect prostate cancer at an earlier stage and potentially save lives, according to new University of Dundee research.
The accuracy of prostate-specific antigen (PSA) screening can be improved by including genetic factors that cause changes in PSA levels not associated with cancer, according to a multi-center study.
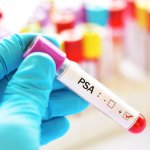
Experts argue that shared decision policies between patients and their doctors have led to high rates of PSA testing and clear medical harm, with minimal benefit and inequity.

Like the better-known prostate-specific antigen (PSA), prostate-specific membrane antigen (PSMA) is a biomarker that can tell physicians much about a patient's metastatic prostate cancer.

A new clinical trial has shown that men diagnosed with prostate cancer can benefit from ‘radical radiotherapy’ that delivers treatment in five hospital visits instead of the typical 20.
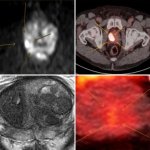
An advanced imaging method is showing promise as a way to improve the diagnosis of prostate cancer by giving clinicians a clearer view of suspected tumours during biopsy.

Researchers demonstrate a HoloLens AR system that enables accurate, flexible needle guidance for transperineal prostate interventions such as biopsy, focal laser ablation, and brachytherapy
Researchers have developed a new blood test to detect prostate cancer which displays greater accuracy than the current prostate-specific antigen (PSA) method.
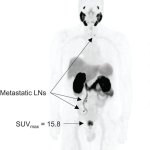
In men recently diagnosed with intermediate or high-grade prostate cancer, PSMA PET/MRI can successfully determine whether their cancer is likely to return within two years of a prostatectomy.

An advanced radiotherapy technique can be used to safely treat prostate cancer patients in as little as one to two weeks, compared with the current standard, which takes one to two months.
A new randomized study confirms that men with high-risk prostate cancer can be treated with a moderately shortened course (5 vs. 8 weeks) of radiation therapy.

Focal treatment of prostate cancer involves treating only the tumor and not the entire gland, sparing surrounding tissue and nerves. The method is being evaluated in a research study.